
Ok. Sure. Of course we do. But the long waits we've recently seen at charging stations are not due solely to an insufficient number. Let's take a deeper look.
First, as EV owners know, the vast majority of us charge at home the vast majority of the time. For most, we only need public charging stations on long trips. As an EV-only household for the last four and a half years who does a lot of long trips (3 350-mile trips a month and 4 or 5 1500- mile trips a year), we didn't see the problem - until recently.
Being retired, we can usually choose when we travel so until this holiday season, we never travelled close to a holiday. On most of our trips, we rarely saw another EV charging at a high-speed charging station. But over Thanksgiving and Christmas holidays, we needed to do 1500-mile trips close to peak holiday travel times. It was a definite wake-up call. We had to wait. A lot.
Of the three to four stops we made in each direction on both trips, there was only one where we didn't have to wait. Fortunately, people were polite and waited their turns. In one case, where we needed a 5-minute charge to make it to our next stop, a slow charging Kona let us jump ahead. He admitted that he needed 45 minutes to an hour to charge and could certainly give us 5 minutes (if we weren't trying to fool him). As it turned out, we disconnected in less than 4 minutes and were on our way, much to his surprise.
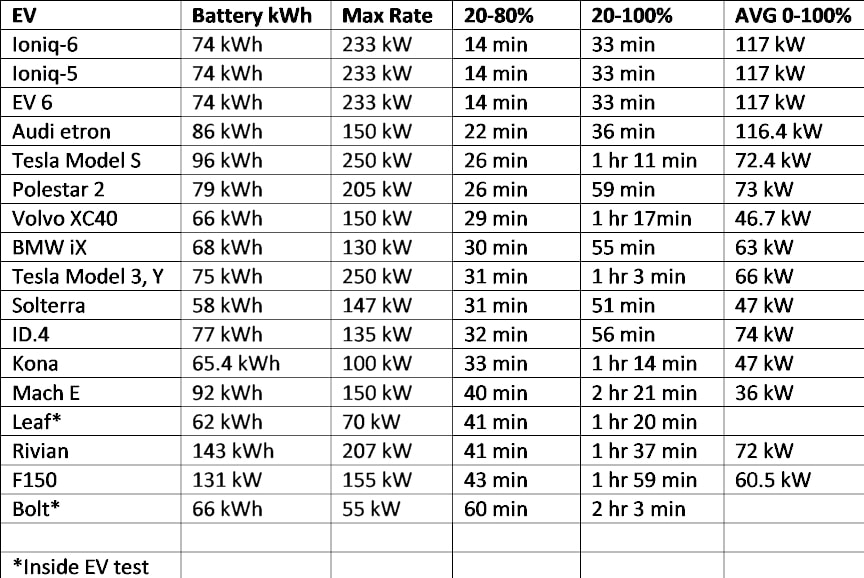
So what was that about? Take a look at this chart of EVs we encountered on our recent two 1500-mile trips. Although we didn't encounter Teslas, I included their charging times just to show how non-Tesla EVs stand up. The numbers come from evkx.net, an excellent site for looking at the performance and charging speeds of pretty much every EV on the market. Since the Bolt and the Leaf are no longer sold, I used numbers from InsideEVs for them.
Of course everyone has a right to charge wherever they want. But for those of us with EVs near the top of the chart, it's pretty frustrating to wait knowing we'd only need 20 or so minutes to charge and could then move on for the next EV. Clearly, you can't blame the EV owners. So who should we blame? How about the manufacturers?
Unfortunately, the manufacturers and many EV buyers look only at max charging speed. But look at the Teslas. They can charge at up to 250 kW, but their charging curves are such that they're pretty far down the list in terms of total charging times.
And if you consider charging past 80%, wow! For almost all of the EVs in the list, it's a disaster and people waiting may get very frustrated.
One more anecdote:
On our way back, since a nearby EA station was full, we decided to try one of the new EVgo stations that advertised 350kW rather than wait. Sure enough there was one charger open of the six on site so we plugged in. It advertised 100 kW and we figured we'd need to charge 25 minutes instead of 15. Unfortunately, we only saw 50 kW. It turns out that the EVgo stations are shared. So, if there are two cars on a station, each will only get half the rated kW.
Nearby, there was a 350 kW station. A Rivian was plugged into one port and was happily charging at 140 kW. Next to the Rivian was a Mach-E. It was charging at 12 kW. It was at 82% so I asked the driver if he was planning to continue charging.
"I have every right to charge!" he shouted, clearly angry that I'd even asked.
"Well, you're only charging at 12 kW on a 350 kW charger. Would you consider trading with us? We'll be gone in 15 minutes."
He rolled up his window and ignored me.
Fifteen minutes later he left and fifteen minutes after that, so did we.
Okay. Bottom line. We need more charging stations and they need to be reliable, especially on heavily travelled weekends and holidays. But, if EVs charged faster - didn't have the major taper we see in most EVs, the throughput at charging stations would be much greater. You'd be back on the road faster and the station operator would make more money (more kWh sold).
If you have a slower charging EV, do consider letting someone waiting jump ahead and if available nearby, definitely think about using a slower charger if your EV can't charge at the higher rates. But better yet, complain to your manufacturer. You don't need faster instantaneous rate; you need faster total charging time. It'll make your trip faster and will reduce the wait times at charging stations.


























































































































 RSS Feed
RSS Feed